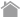Various non-specific reactions of antibodies
Non-specific reactions should always be considered even if the data seem clear.
Non-specific reactions can make truly negative samples look positive (false positives) and truly positive samples look negative (false negatives).
Main causes of non-specific reactions of antibodies
・Fc receptors
・Non-specific reactions of a secondary antibody
・Heterophilic antibodies
・Rheumatoid factors
Fc receptors
False positive signals may occur when samples (cells and tissues) express receptors for the Fc portion of the antibody molecule (Fc receptors).
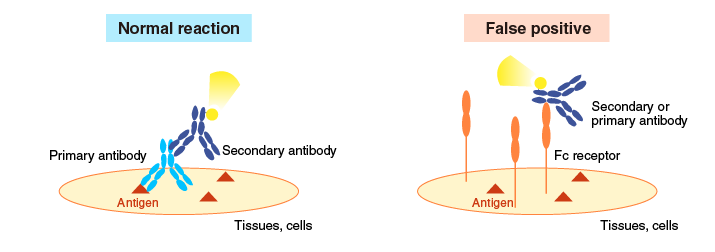
Non-specific reactions of a secondary antibody
Secondary antibodies are selected based on the species of animal used to generate the primary antibody. When using a polyclonal secondary antibody, a portion of the secondary antibody may react with proteins of other animal species.
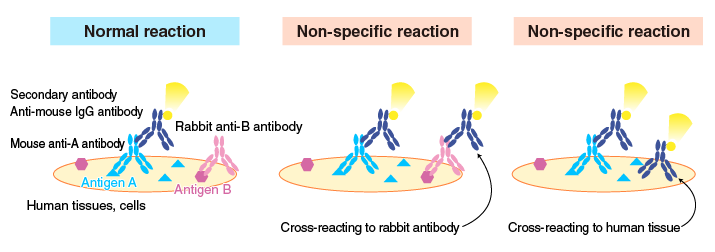
Heterophilic antibodies
Human blood sometimes contains antibodies that bind to mouse antibodies. These antibodies are called human anti-mouse antibody (HAMA). Antibodies that react with antibodies of other animal species include goat (HAGA), sheep (HASA), and rabbit (HARA) antibodies.
These antibodies are collectively called “heterophilic antibodies”.
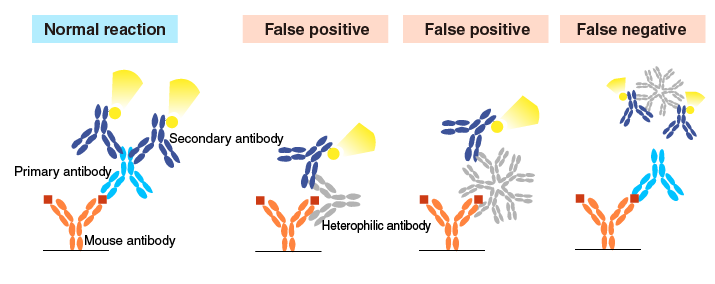
The exact reason for the presence of heterophilic antibodies is unknown. HAMA can be found in a significant proportion of healthy individuals who have never been exposed to mice.
Rheumatoid factors
 Human blood may contain antibodies that react with human antibodies. A well-known example is autoantibodies commonly found in patients with rheumatoid arthritis. They are typically IgM-type immunoglobulins specific for the Fc fragment of human IgG and called rheumatoid factors (RFs).
Human blood may contain antibodies that react with human antibodies. A well-known example is autoantibodies commonly found in patients with rheumatoid arthritis. They are typically IgM-type immunoglobulins specific for the Fc fragment of human IgG and called rheumatoid factors (RFs).
Although RFs are directed against the Fc fragment of human antibodies, they also react with antibodies of other species, causing false positives/negatives in tests that use mouse antibodies.
In antibody-based clinical tests, interference from RFs in the samples should not be ignored, because RF levels are high in a few percent of rheumatoid arthritis patients and healthy individuals, and in about ten percent of the elderly. False reactions do not only reduce the reliability of the test, but also endanger the lives of misdiagnosed patients.